Center for Global Surgery
Through multidisciplinary and bidirectional partnerships, innovation, education, and policy advocacy, we aim to improve access to essential surgical care by addressing the barriers to such care by training the next generation of global health leaders and building sustainable capacity in regions with health inequities.
Approximately 5 billion of the world’s 7 billion people have no access to safe, affordable surgical and anesthesia care, resulting in more deaths and disability than HIV/AIDS, tuberculosis and malaria combined. Misconceptions as to the cost, required supplies, expert knowledge and scope often serve as obstacles to offering surgical relief to many patients in low-resource areas in low-, middle- and high-income countries. Addressing surgical disparities and issues surrounding access to care is of paramount importance, as untreated disability caused by degeneration, non-communicable diseases or trauma is often a death sentence in these environments.
The Center for Global Surgery houses and strengthens the multidisciplinary initiatives that are ongoing in global surgery at Northwestern, funded through grants, donations and NGOs.
Center Leadership
Featured Projects
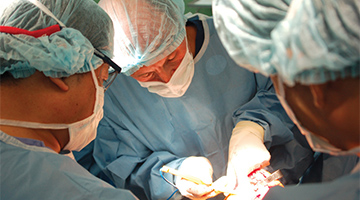
Neonatal Nutrition and Outcome Assessment
Northwestern Faculty: PI Monica Langer, MD
Neonatal mortality is an increasing cause of under-5 deaths in low-income countries (LICs). Surgical congenital anomalies such gastroschisis, esophageal atresia, and intestinal atresia are among the most lethal neonatal conditions, with 30-day mortality ranging from 60-85% in Uganda. These anomalies prevent oral/gastric feeding until recovery after surgery but delays in presentation and access to surgical care mean these babies often have to wait 10 – 20 days to be fed. Newborns deplete nutritional reserves within 5 days, consequently, severe malnutrition and electrolyte disturbances result in poor healing and high mortality.
Through this study, nutritive enema feeding (NEF) is proposed as a perioperative nutritional "bridge" until these babies can feed by mouth. NEF has successfully nourished adults, prior to development of IV fluids/PN, and recently fed two infants after intestinal resections in Sweden and Nepal. Similar to absorption of suppository medications, NEF extends this to enema delivery of breastmilk with lactase as a cheap, developmentally appropriate nutrition source.
Dr. Langer has been working to evaluate baseline characteristics, peri-operative morbidity, growth, enteral feeding tolerance, and mortality in surgical neonates in Uganda and build research capacity in the Pediatric Surgery team at Mulgao National Referral Hospital (MNRH).

Obstetric Fistula Repair
Northwestern Faculty: PI Stephanie J. Kielb, MD
Due to obstructed labor, or attempts to relieve this labor via cesarean section, fistulas cause devastating injuries for women, like total urinary and/or fecal incontinence. Women are often ostracized from their families and communities and unable to access safe, affordable surgical care.
Since 2012, Kielb has worked twice a year in Kigali, Rwanda, at Kibagabaga Hospital to repair obstetric fistulas for women with the International Organization for Women and Development. Her team works closely with the Rwandan Ministry of Health, local staff at the Kibagabaga Hospital and Rwandan surgeons. They keep detailed records and charts with regular reporting of outcomes to the Ministry of Health and quality improvement metrics in place for optimal patient care.
The team trains Rwandan medical students and residents and includes educational programs intended to prevent fistula formation. Kielb also conducts IRB-approved research in Rwanda, evaluating the regional variation in fistula formation, the change in trends as to the cause of fistula and the importance of intra-operative cystoscopy during fistula repair. These projects involve Rwandan medical students, residents and physicians, as well as Northwestern students and residents.
Kielb also serves as a board member and mission leader for the International Organization for Women and Development.
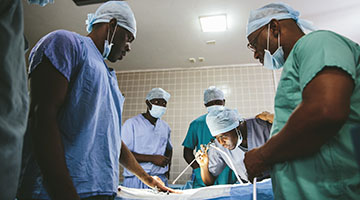
Project BURST: Building Urologic Research and Surgical Training
Northwestern Faculty: PI Adam B Murphy, MD
Murphy's team, in collaboration with the chief of surgery and fellow urologist Dr. Edet Ikpi, implemented basic infrastructure to integrate urology education into the surgical residency curriculum at the John F. Kennedy Hospital in Monrovia, Liberia, to embark on bidirectional educational exchange and future research endeavors. The hospital has been sent biomedical equipment, surgical instruments and educational materials.
The collaboration is funded in part by the World Bank to expand urologic surgical training. Ikpi, who trained at the University of Calabar Teaching Hospital in Nigeria, collaborated with Murphy on an evaluation of prostate cancer in Nigeria by looking at autopsies, funded by the Northwestern Global Health Catalyzer Grant.
Through the collaboration and guidance of the Northwestern team, Ikpi was responsible for the department achieving regional accreditation by the West African College of Surgeons for their surgical residency training program.

RISE Initiative
Northwestern Faculty: PI Sumanas (Sue) Jordan, MD, PhD
As a part of the RISE Initiative, the Gender Pathway Program takes a multidisciplinary approach to provide self-empowering and self-affirming psychological, medical and complex reconstructive care to the transgender, gender-expansive and victims of female genital cutting community.
Female genital cutting, a traditional, non-religious or cultural practice harmful to young girls and women, comprises all procedures that involve partial, or total, removal of the external female genitalia or other injuries to the female genital organs for non-medical reasons. This practice is currently increasing in high-income countries while it is decreasing in low-income countries.
Jordan's team strives to create a secure, safe atmosphere for patients and aims to advocate for gender and sexual minorities and victims of female genital cutting.
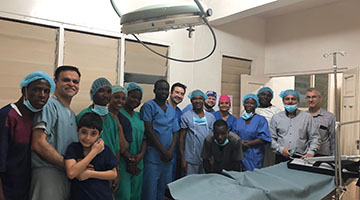
Pediatric Global Surgery Program
Northwestern Faculty: PI Fizan Abdullah, MD, PhD
Building surgical capacity and evaluating the quality of care in Sub-Saharan Africa are the two focuses of Abdullah’s team in partnership with Dr. Hope Addy of Korle Bu Teaching Hospital in Accra, Ghana. On a recent trip to Accra, the team taught the Fundamentals of Laparoscopic Surgery over two days to a group of surgeons from three different countries with standing room only.
The team then traveled to Liberia to conduct a two-day course on inguinal hernia repair, a common pediatric surgical problem easily corrected with appropriate surgical training. These efforts to train local surgeons have the potential to expand access to surgical care multifold in under-resourced areas.
Research fellows at Ann & Robert H. Lurie Children’s Hospital of Chicago have active lines of inquiry examining children’s access to surgical care, the quality of existing surgical care and the ease of implementation of novel database registries. These registries allow scientists to understand longitudinal patient outcomes and assess baseline characteristics of developing surgical systems around the world. Discussions about implementing a novel database registry are underway in Zambia.
Resources
The Global Surgery Steering Committee
The Global Surgery Steering Committee’s inaugural meeting was held on March 31, 2016. Brought together by David Stulberg, MD, and Vicky Brander, MD, eight surgeons and physicians met to learn about surgical initiatives at Northwestern Medicine and to determine constructive ways to support individual and collective efforts. The Steering Committee also served as the initial advisory committee for the Center for Global Surgery.
- Fizan Abdullah, MD
- Sam Attar, MD
- Victoria Brander, MD
- Roxanna Garcia, MD
- Wilson Hartz, MD
- Eric Hungness, MD
- Stephanie Kielb, MD
- Magdy Milad, MD
- Adam Murphy, MD
- Steven Schuetz, MD
- Nathaniel Soper, MD
- Sam South, MD
- Samuel Stulberg, MD
- Jonathan Vacek, MD


